

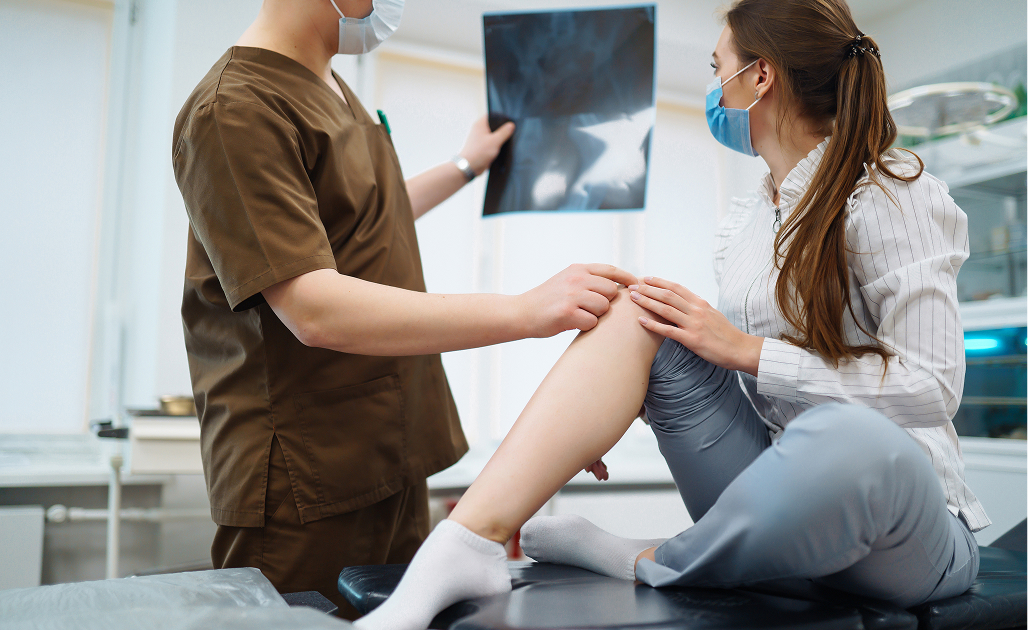
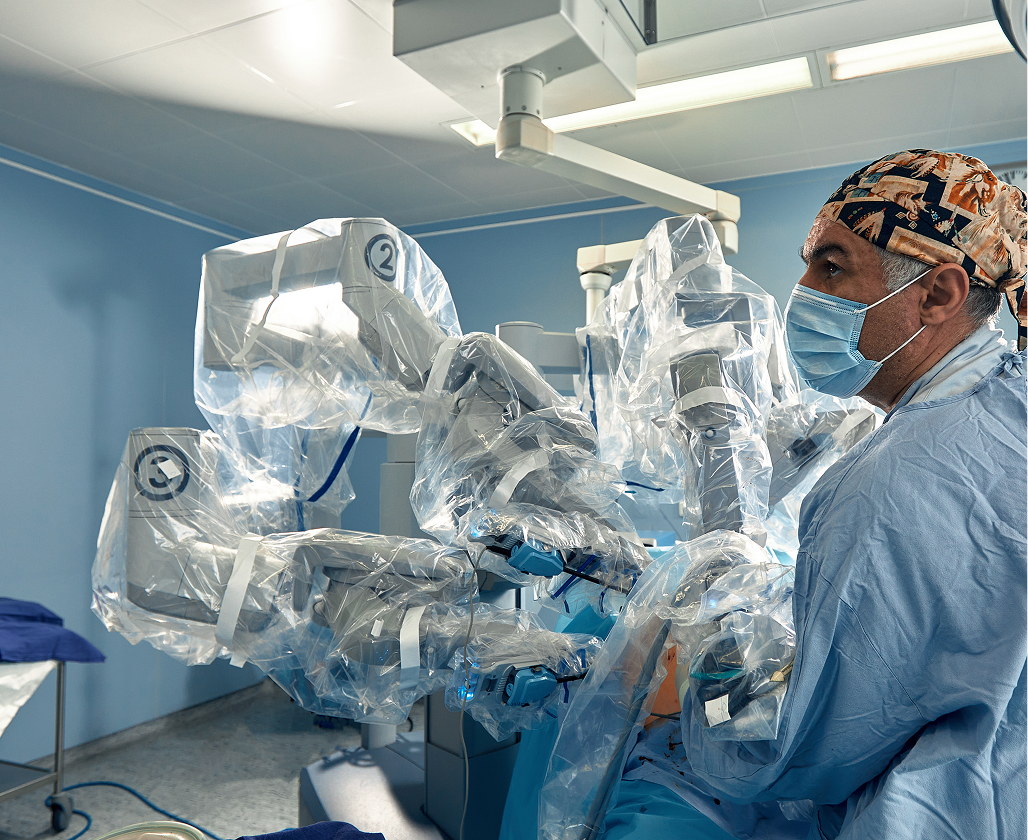
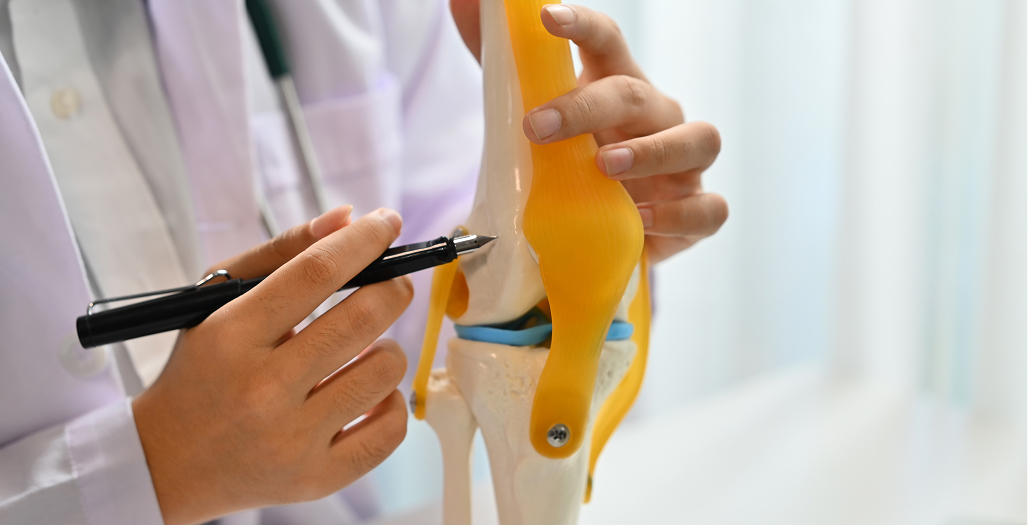
If you are considering knee replacement and wish to explore whether robotic-assisted surgery could offer advantages for your specific condition, the first step is a comprehensive consultation with Dr Richard Allom.
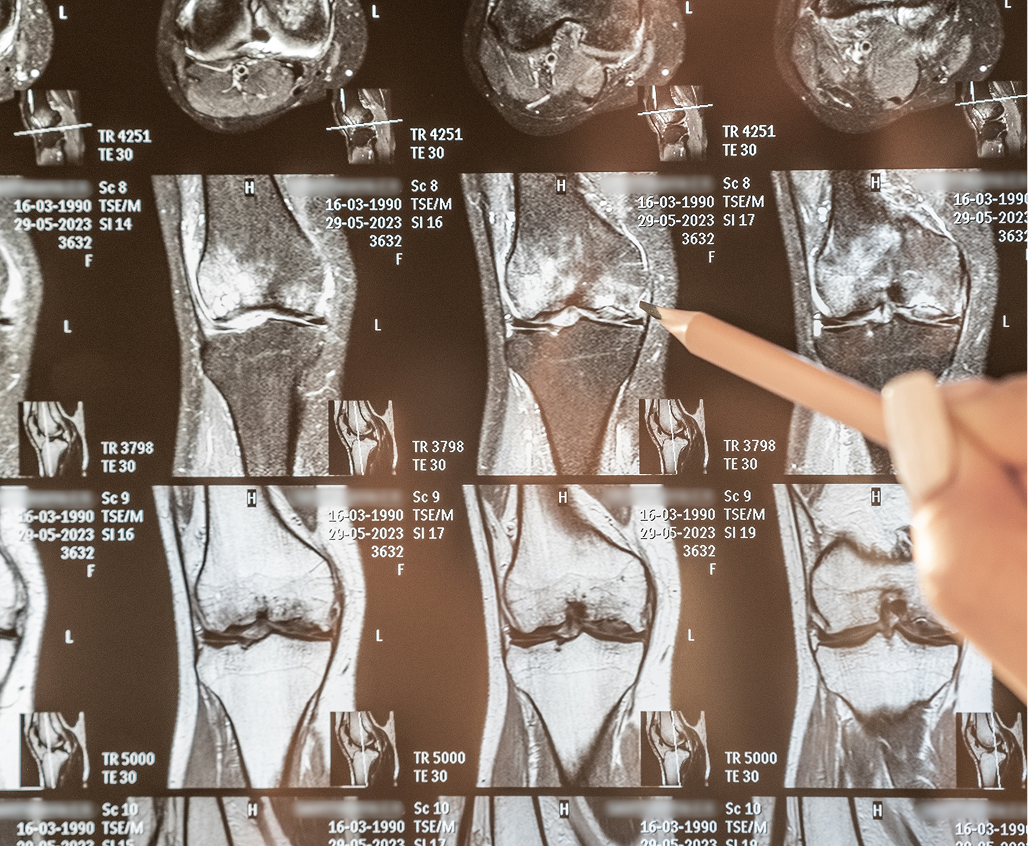
What to Bring: Please bring your referral letter, all relevant imaging studies (X-rays, CT scans, MRI if performed), and your list of current medications to your consultation.