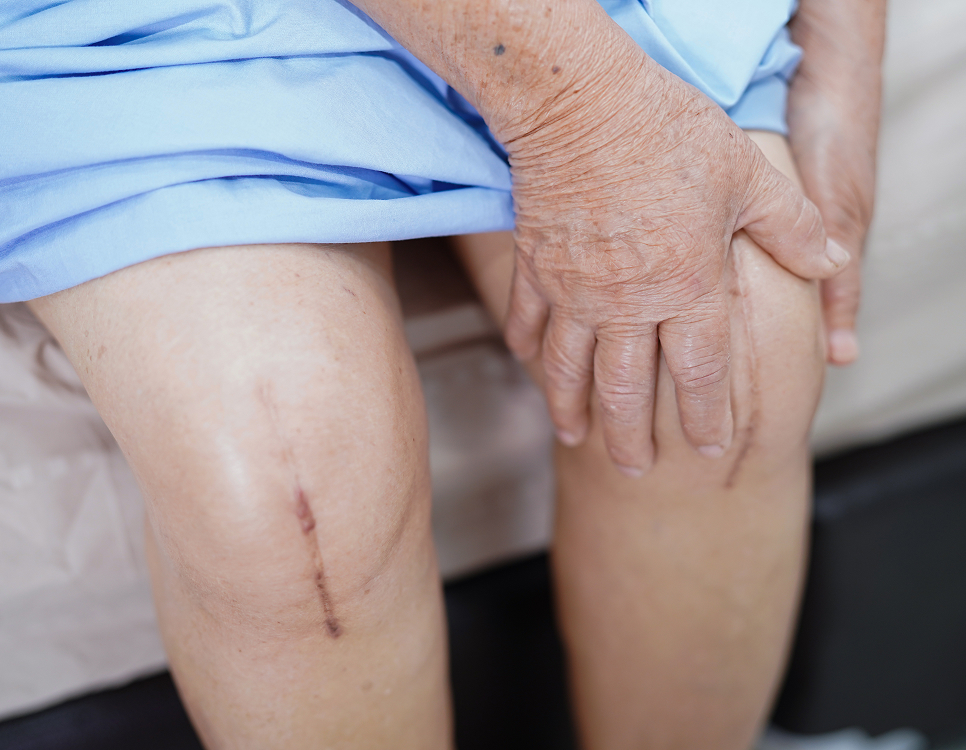
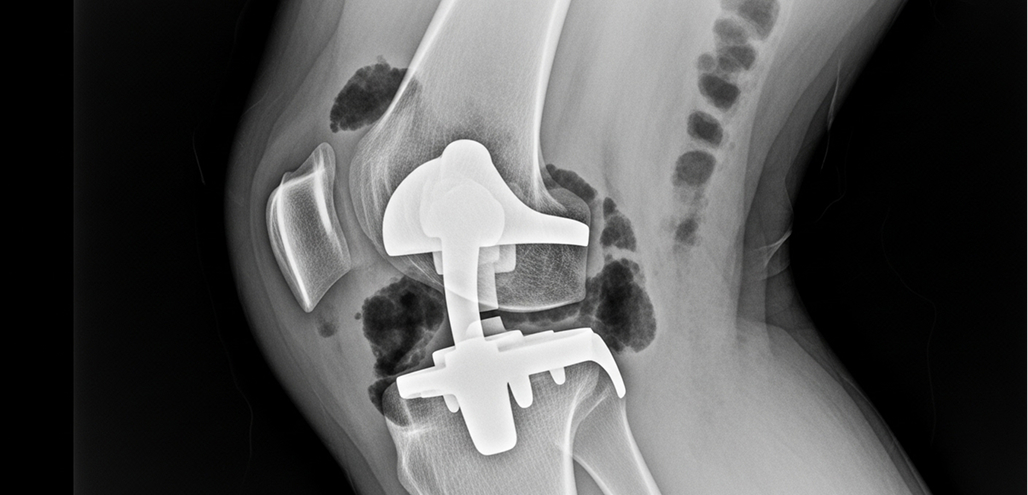
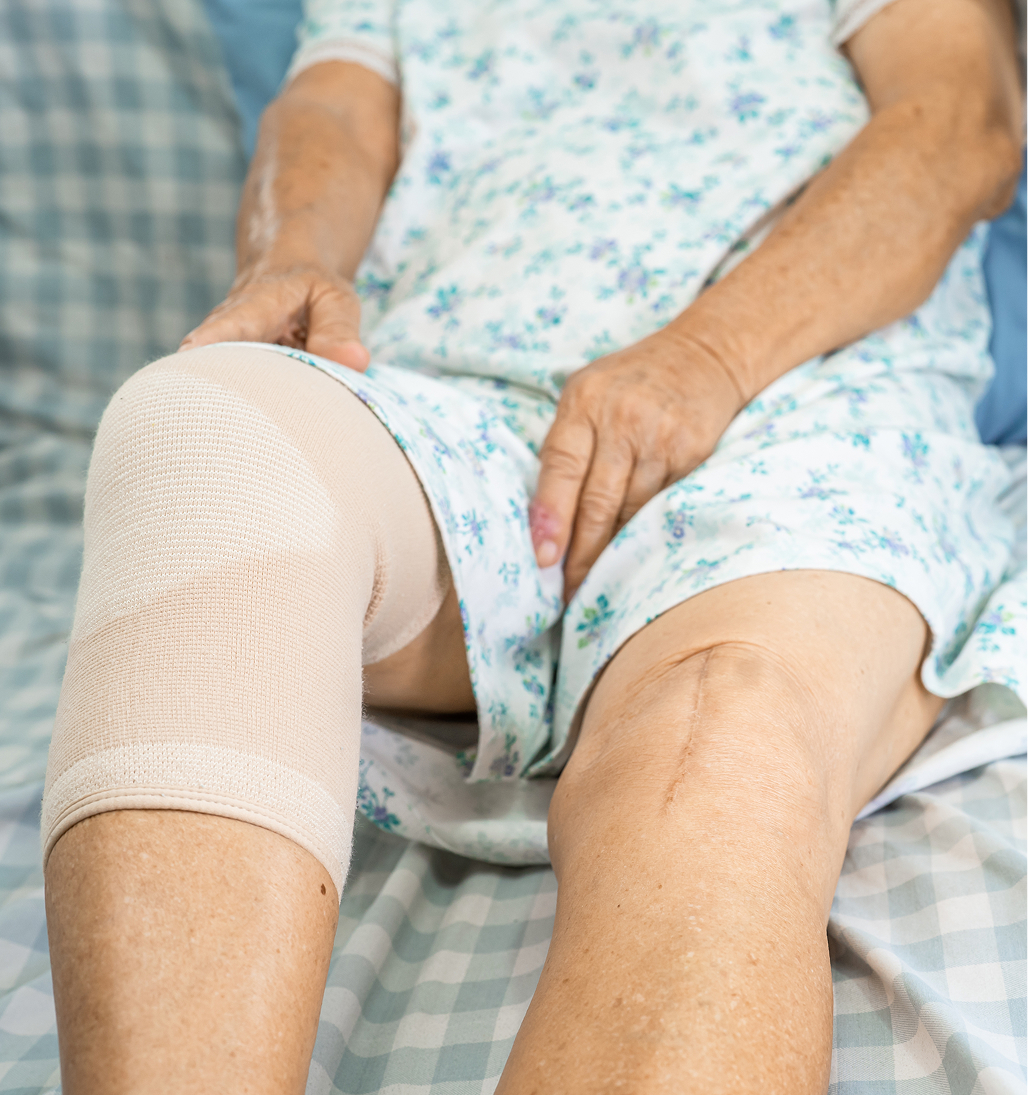
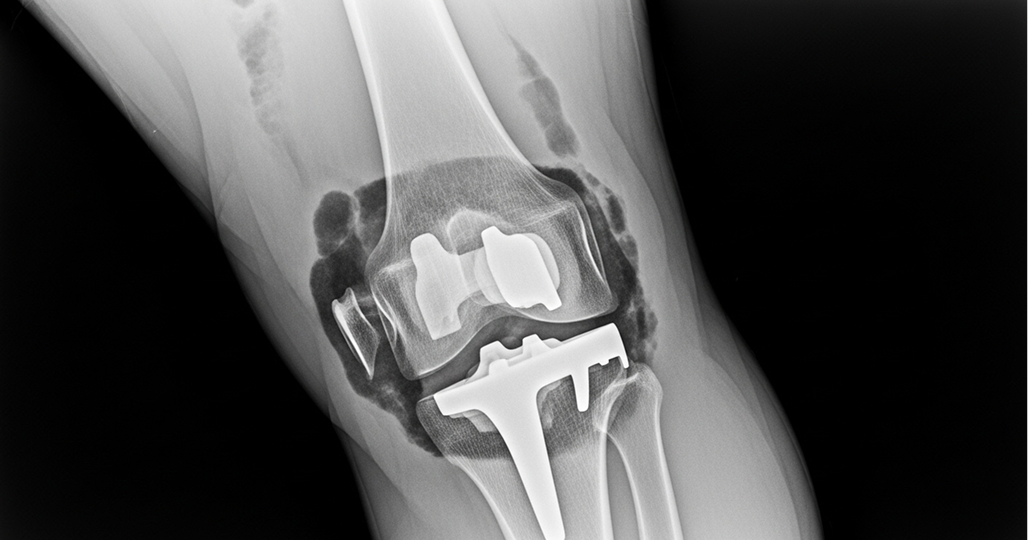
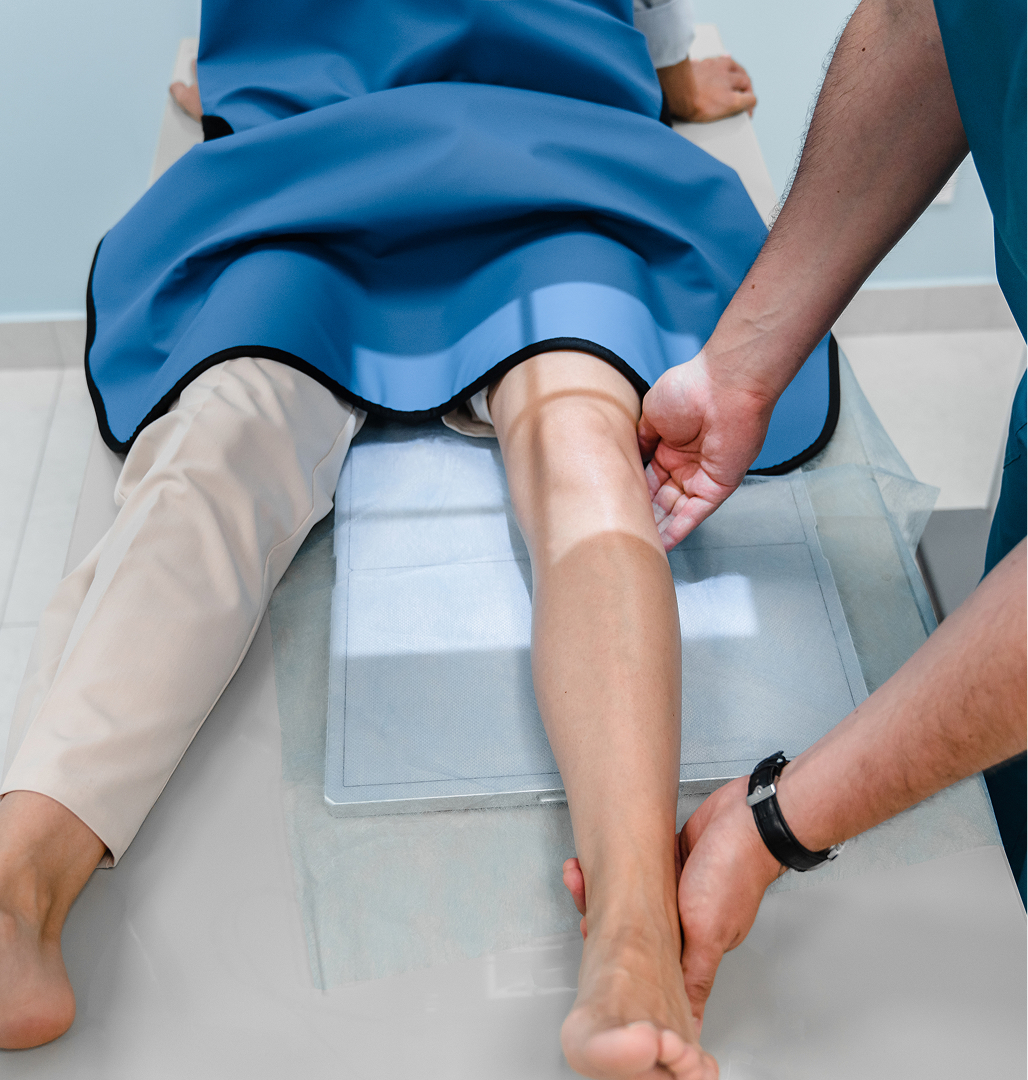
Revision knee replacement aims to remove the failed implants, correct the underlying problem (like loosening, instability, or infection), address any bone loss, and implant new, specialised revision components.
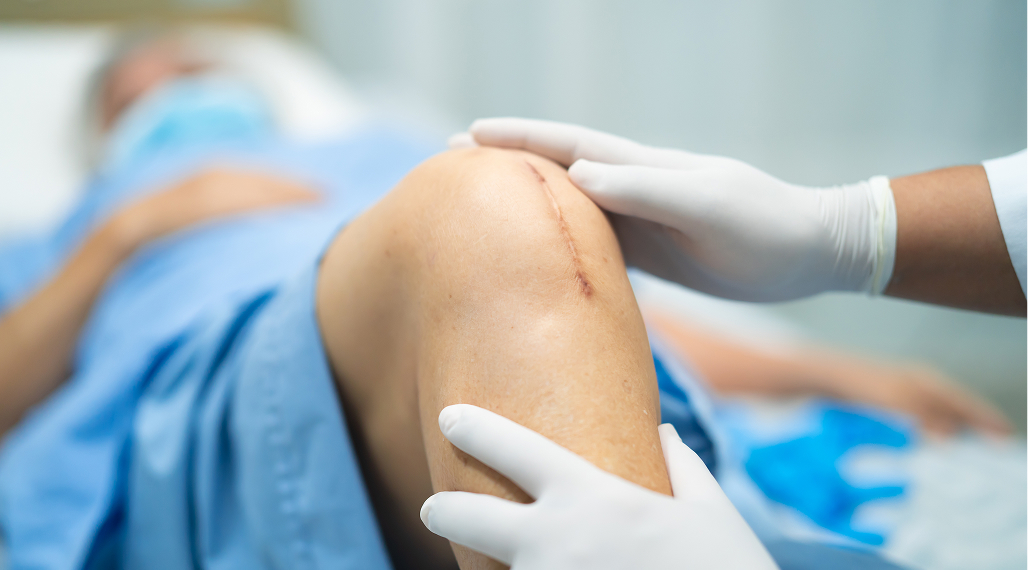
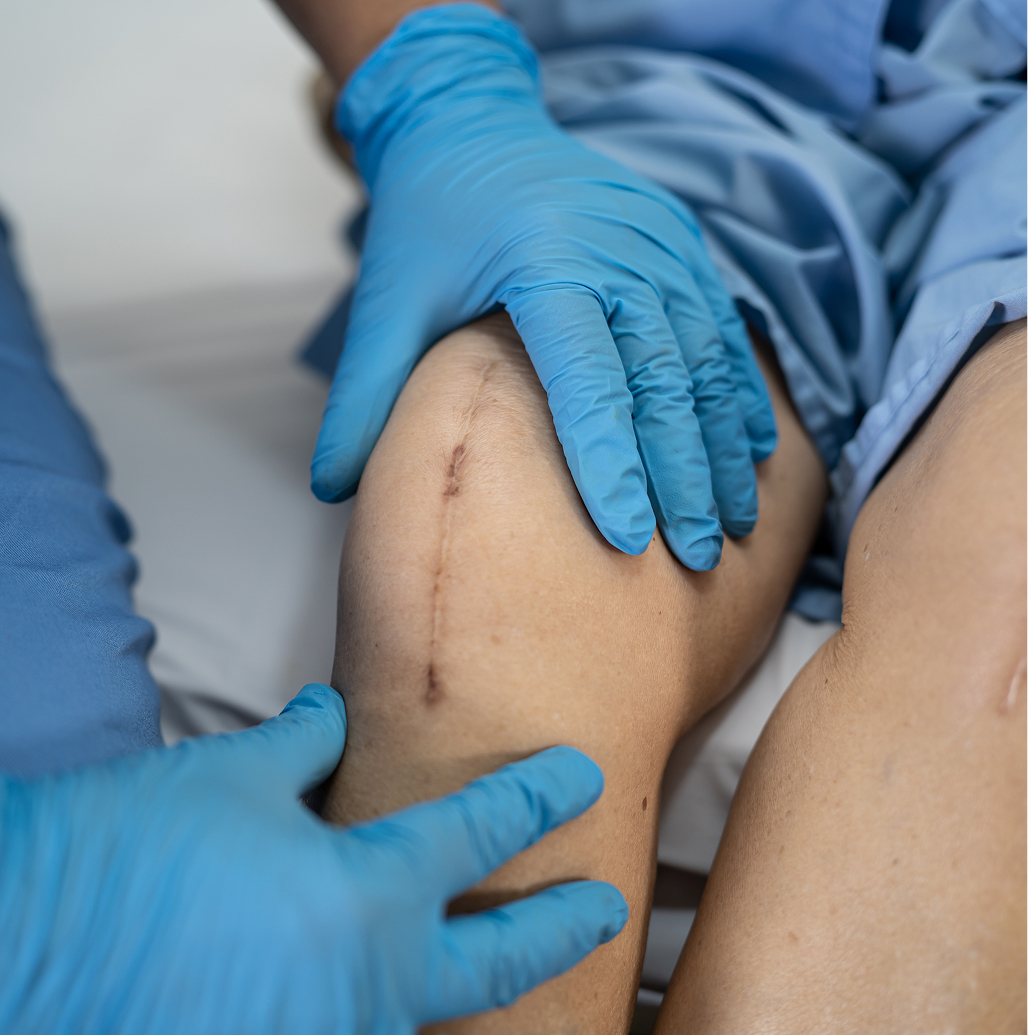
Yes, in most cases. Revision knee replacement surgery can address the reasons for failure and provide significant pain relief and improved function. Success depends on identifying the cause, having enough healthy bone, stable soft tissues, no active infection, and good overall patient health. With subspecialist expertise, even complex situations can often be successfully managed.
Yes, revision surgery generally carries higher risks. Potential complications like infection (3-5% vs 0.5-1%), instability (3-8%), fracture (2-4%), nerve injury (1-2%), and stiffness (5-10%) are more common than with primary surgery. However, experienced subspecialist surgeons use specific techniques and careful planning to minimise these risks.
A knee replacement can technically be revised multiple times. But each subsequent revision becomes more difficult due to increasing bone loss, scar tissue, higher risks, and potentially less functional improvement. The goal is always to make the current revision surgery the definitive, long-lasting solution if possible.
Often, a revision knee doesn't feel quite the same as a perfectly functioning primary replacement. This can be due to bone loss, scar tissue, or the need for more constrained implants. However, the main goals – significant pain relief and improved function for daily activities – are achieved for most patients. Expectations should be realistic; the aim is a good functional outcome, though perhaps not perfection.
Revision implants generally have good longevity, though perhaps slightly less than primary implants. Studies show around 85-90% survival at 10 years for revisions done for loosening without infection. For revisions due to infection, survival rates are slightly lower, around 75-80% at 10 years. Longevity depends on factors like bone quality, implant type, activity level, and the reason for revision.
Feeling anxious about another surgery after a previous one failed is completely normal. Concerns about risk, recovery, or potential for another failure are common. It's important to remember that non-surgical options for a failed replacement are usually ineffective long-term, and ongoing problems can worsen bone loss. I am committed to discussing all risks and benefits transparently, setting realistic expectations, and ensuring you feel fully informed and supported in your decision. Seeking a second opinion is always welcome.
If you have ongoing pain, instability, or difficulty with function after a knee replacement, a subspecialist assessment is the first step towards finding a solution.
Please bring your referral letter, all relevant imaging studies (X-rays, CT scans, MRI if performed), and your list of current medications to your consultation.